This is a series! Make sure you start at Part 1!
What Kidney Failure Actually Looks Like
I want to start with a man I knew, a man in his early seventies, close enough to my own age that there was no safe psychological distance between his life and mine. He was an old man, strong and handsome, mentally sharp, and fully aware of what was happening to his body, and clear-eyed about what his life had become after years of listening to and following medical “management.”
He had been on dialysis for nearly fifteen years, and those years did not represent treatment followed by recovery. They represented a slow narrowing of his world until almost everything revolved around getting to and from a dialysis center and surviving what those sessions took out of him.
Several days each week were consumed by hours hooked up to a machine that pulled his blood out of his body, ran it through an artificial filter, and pushed it back in again. By the time the session ended, he was exhausted in a way sleep did not fix. He felt cold, lightheaded, nauseated, and weak. Whatever plans existed for that day were usually abandoned, and the following day was spent trying to recover enough strength to function before the cycle began again.
Travel became unrealistic. Being gone for more than a short window meant missing treatment, and missing treatment meant paying for it physically. Spontaneity disappeared.
He had a family who loved him and wanted him present. Children who still wanted time with him. Grandchildren who were growing quickly and wanted to know their grandfather while he could still engage with them. They wanted to travel together, see the world, and make memories that did not involve hospital rooms and treatment schedules.
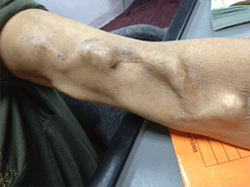
Before dialysis ever begins, there is the fistula, a word that sounds tidy and benign until you understand what it actually means: a page out of Frankenstein’s how-to manual. Surgeons permanently alter circulation in the arm by connecting an artery directly to a vein so it can withstand repeated punctures with large needles. The vessel enlarges unnaturally, the arm changes shape, and the skin stretches over something that visibly throbs and vibrates. You can feel it buzzing under your fingers.
That fistula is accessed again and again, week after week, year after year. Thick needles are inserted each time. Scar tissue builds. The arm becomes tender, then numb, then distorted. Bleeding is a constant risk. Patients learn to protect that arm instinctively because losing it means losing the ability to continue treatment at all.
As his kidney function continued to fail, his body began to swell. Fluid accumulated because it could no longer be filtered and removed effectively. It started in his legs and ankles and gradually moved upward. His skin became tight and shiny. Eventually, fluid began to leak through the skin itself because there was nowhere else for it to go. Breathing became harder as fluid backed up into the chest, creating a constant sense of air hunger that never fully eased.
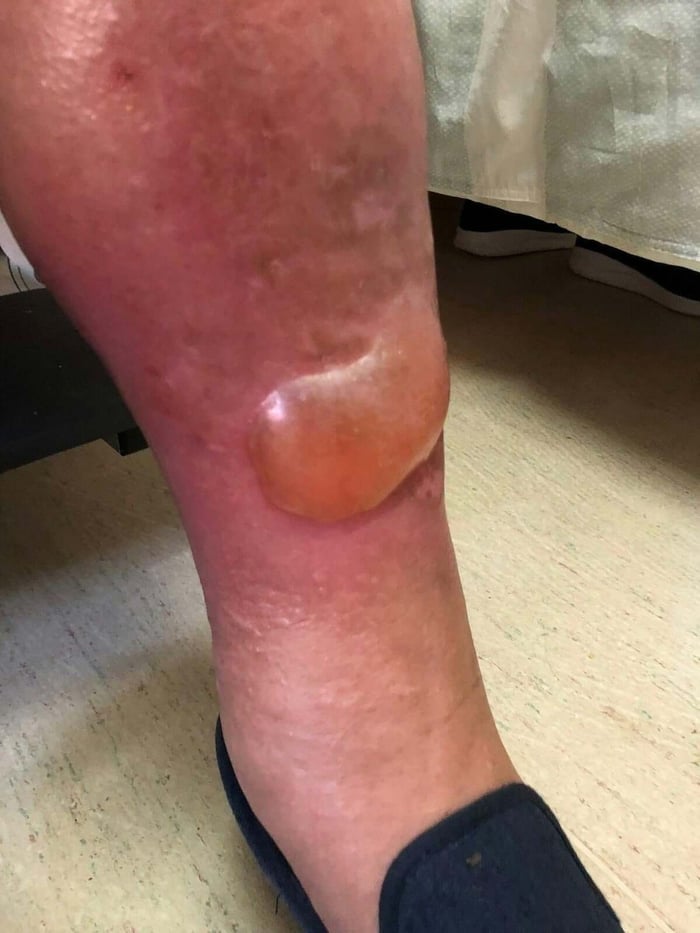
This is what kidney failure looks like when it progresses far enough. It is not an abstract diagnosis or a laboratory trend. It is a body that can no longer move fluid or waste, a person becoming heavier, more uncomfortable, and more exhausted as each day passes. Doing this to a person is unconscionable.
Eventually, he reached a point where he decided he had had enough. He understood exactly what that decision meant. He knew that stopping dialysis would end his life, but he also knew that continuing meant spending whatever time he had left tethered to a machine that kept him alive but sick, weak, and increasingly miserable. He chose to stop because the life he was sustaining no longer felt like living. Can you imagine what it would feel like to make a decision to end your life and die a horrible, painful death?
I have watched this decision made countless times, and it never comes from confusion or ignorance. It comes from clarity. It comes from understanding exactly what the future holds.
Watching someone reach this point forces a question that medicine rarely asks honestly. How did so many people end up here after years of being told their disease was controlled, their numbers were better, and their risk was being managed? How did patients whose blood pressure had been treated for years arrive at a place where their kidneys failed so completely that survival itself became intolerable?
It was Never about the Heart
Kidney failure does not appear out of nowhere. It is the endpoint of a long process, and in many cases, that process includes years of interfering with the very pressure the kidneys require to do their job.
Before we talk about numbers, drugs, or guidelines, we have to be honest about the outcome. This is what is at stake when blood pressure is treated as an enemy rather than a signal from the filters we call kidneys.
What almost no one tells patients is that what we call “blood pressure” has nothing to do with the heart. It is a downstream measurement that largely reflects the force required to push blood through the kidneys so dynamic filtration can occur. Meaning it MUST fluctuate depending on the current circumstances. What we are measuring in the arm is not a cardiac defect. It is the pressure the system is generating to meet renal demand. It is therefore kidney pressure, not blood pressure we should be thinking about. Therefore, looking to the kidneys and the primary root cause and supporting the renal system, not the cardiac system.
The heart is not setting this number in isolation. The heart responds directly to the kidneys’ demands.
Kidneys are filters that require force. When filtration becomes harder, whether because of dehydration, thick waste-filled blood, vascular wall constriction, increased waste load, or long-term structural damage to the filter systems, the body raises pressure to keep waste moving out of the bloodstream. That increase in pressure is not a mistake. It is a compensatory response meant to preserve life. Imagine, at this point, thinking that drinking the waste products of your blood is a health elixir. Read my 4-part series titled “God’s One Mistake” about how drinking your own piss is devastating to your renal system and other stupid things I have to say to adults.
By focusing on the heart and treating the pressure itself as the disease, the medical industrial complex has mistaken the messenger’s sound for the problem. It is not even the messenger we are fixated on, but the clothes the messenger is wearing. Can you see how far off the mark this is? Lowering the number without restoring the kidney’s filtering capacity does not fix the system. It removes the force the kidneys were relying on to function at all. So your blood pressures are low, and the cardiologist can prance around the room shouting victory as he silently sentences you to a possible fate worse than death. But we can’t fault them, right? After all, they have a new vacation home to think about, and those mortgages don’t pay themselves.

This is why patients can have “well-controlled blood pressure” while their kidney function quietly deteriorates. We are not looking at the right end of the horse.
What we are really observing when we take a blood pressure reading is kidney pressure expressed through the vascular system. We squeeze an artery in the arm, listen for turbulence, and assign meaning to the heart, when the real question should be: why did the kidneys need that high pressure in the first place?
When pressure is chronically suppressed without addressing renal demand, perfusion falls, filtration slows, waste accumulates, and fluid backs up. Over time, the body pays for that decision. The swelling, the fluid overload, the shortness of breath, and eventually dialysis are not mysterious complications. They are the predictable outcome of interfering with compensation while ignoring the cause. When I worked in the field, I would call patients’ edema “Amloda-Legs” referring to patients who took amlodipine and would have horrible swelling in their lower extremities that was unmistakable. It was either amlodipine or drank the highly addictive Ensure meal replacement shakes made with the same ingredients as final phase hog feed. Read more about that in my ebook Food Fornifaction: They’re Fucking with Our Food. Quote from my book:
_________________________________________________________
According to nationwide surveys conducted by the National Institutes of Health, nearly 70% of adults in the U.S. are either overweight or obese. Let that sink in. This is not a percentage that can be solely explained by eating too much and exercising too little. Since the early 1960s, U.S. obesity rates have tripled, and morbid obesity has risen tenfold.
_________________________________________________________
If the goal is to preserve health rather than manage numbers, then blood pressure cannot be treated as a root problem. It is the signal’s sound. The root lives downstream, in the kidneys, in vascular tone, and in the conditions that make filtration compromised in the first place.
White Coat Hypertension Is Not a Fluke
White coat hypertension exists because the kidneys do not operate in isolation. They sit directly beneath the adrenal glands, which are environmental response organs. They sit like little hats on top of the kidneys. They are survival glands designed to read the room before the brain puts a spin on it.
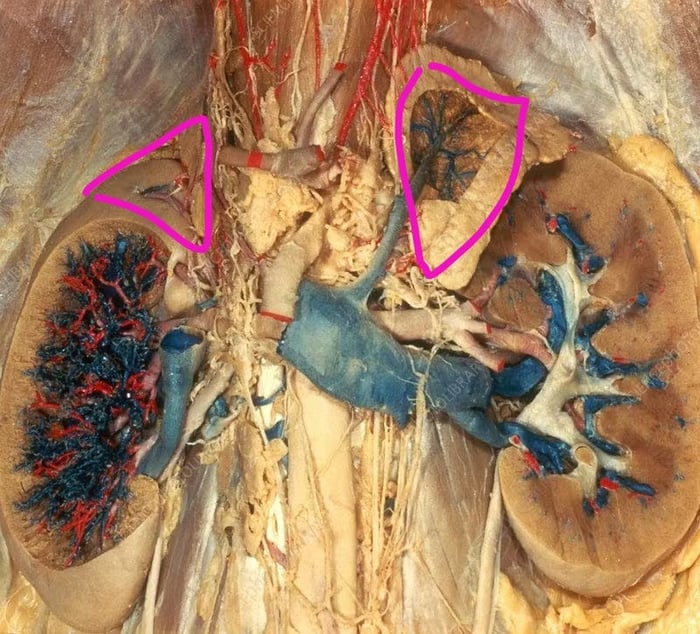
When the environment signals threat, uncertainty, scrutiny, or loss of control, the adrenals respond immediately. They release stress hormones that tighten blood vessels, shift fluid balance, and increase the force required to move blood through the kidneys. This is not a pathology. It is a survival response.
A medical office is not a neutral environment for the body. It smells unfamiliar. It is brightly lit. It is quiet in a way that is overtly surveilled with a sense of impending doom. A cuff is placed around the arm and tightened until blood flow is restricted. The patient has usually been explicitly told that a bad number means danger. Often, they are already anxious because previous readings have been labeled “high,” “borderline,” or “concerning.”
The adrenals read all of this instantly.
They do not ask whether the threat is real or imagined. They do not care that the danger is abstract. Their job is to prepare the body to meet demand. They signal the kidneys to retain sodium and water, they increase vascular tone, and they raise the pressure required to maintain filtration under perceived stress.
The result is predictable. The number goes up, exactly as the body is designed.
If this were a heart defect, reassurance would not change the reading. If this were a fixed mechanical failure, context would not matter. But context matters profoundly. Calm the patient, slow their breathing, remove the sense of threat, give the system time to settle, and the pressure automatically falls on its own.
That alone should have ended the debate decades ago. But alas, that is not where the profit margins lie. The lie is for the profit margins.
White coat hypertension is treated as a nuisance variable, something to be worked around or corrected for. In reality, it is one of the clearest pieces of evidence that blood pressure is a responsive signal driven by environmental interpretation and renal-adrenal coordination. It proves that pressure is not static, not intrinsic, and not a standalone disease.
The adrenal glands sit atop the kidneys for a reason. Stress hormones directly affect renal blood flow, filtration rate, and vascular resistance. When the environment feels hostile or uncertain, the body prepares to conserve resources and maintain internal balance under strain. Pressure simply rises because pressure is required.
Instead of asking why a person’s system is responding this way, the elevated reading is often treated as proof of an underlying cardiac condition that needs to be suppressed. A situational response becomes a permanent label. A momentary demand becomes a lifelong, slow kill death sentence diagnosis. Keep in mind how technically coml]plicated dialysis is.
Once medication is introduced, the system is no longer allowed to respond intelligently. The pressure is blunted regardless of context. The adrenals continue to read threat. The kidneys continue to require force to filter.
Why Kidney Damage is Inevitable
Think of the kidneys as an industrial filtration system that only works if the pressure is exactly right. Not too high, not too low. Just right. And we need a valve that reads the ever-changing needs of the system, which are constantly shifting.
Blood arrives carrying everything the body has used and everything it still needs. The kidney does not “clean” blood. It separates it. Sodium here. Potassium there. Calcium handled carefully. Waste pushed out. Water balanced. That sorting only works because blood is being pushed through the filters with enough force to separate what stays from what leaves.
Pressure is the driver of that separation.
If the pressure drops too low, filtration slows. Waste is not cleared. Potassium begins to rise. Sodium handling becomes sloppy. Fluid accumulates. The body swells because there is no longer enough force to move water out of circulation. Electrical signals in the heart become unstable. This is not theoretical. This is how people die quietly from electrolyte imbalance.
If the pressure is distorted long enough, the kidney adapts by sacrificing precision. It holds onto what it should let go of and loses what it should keep. Calcium ends up in vessels instead of bones. Potassium lingers in the blood. Sodium balance collapses. The system holds together until it doesn’t. The body is trying desperately to compensate for the low pressure by raising it to the proper range to filter the backlog.
Dialysis occurs when the filtration system finally fails.
Dialysis does not heal the kidneys. It replaces the once-perfect and finely tuned pressure-driven filtration with an external machine. Blood is drawn from the body, forced through an artificial filter, and returned. That machine exists because pressure inside the body can no longer do the job. Dialysis is the admission that the system has broken the pressure valve beyond recovery.
Here is the part that matters.
Dialysis only works because the machine precisely controls pressure. Too little pressure, and waste is not removed. Too much pressure and blood cells are damaged, electrolytes shift dangerously, and the patient crashes. Even artificial filtration requires tight pressure control to avoid killing the person attached to it.
Now imagine what happens when pressure is chronically altered inside the body without fixing why filtration became difficult in the first place.
Lower the pressure, and the kidney loses the force it needs to sort waste. Raise the pressure without addressing structural damage, and the filters scar and fail. Either way, the outcome is the same. Filtration degrades as electrolytes drift and fluid begins to accumulate. The body compensates by attempting to raise pressure until it can no longer.
Dialysis is the endgame proof. When pressure-driven filtration fails, life can only continue by replacing it artificially. That is checkmate. This is why pressure is not the enemy. Pressure is the requirement for filtration. Changing it without restoring the system that depends on it does not fix the disease. It just guarantees the outcome.
Medications Change the Number, Not the Outcome
Once blood pressure became a diagnosis instead of a signal, medication became the default response, not because it solved the problem, but because it made the number behave. That’s the entire appeal. You can lower it, record it, bill for it, and move on. And what most people don’t recognize is this. The medical industry works with chemicals and how they change something we can measure. IT HAS NOTHING TO DO WITH YOUR HEALTH. They drool savagely over discovering a chemical soup that can change a blood lab value or something they can measure. That is all, the beginning, middle, and end. THEN THEY MAKE UP A STORY TO GO ALONG WITH THE MARKER CHANGE. Like LDL cholesterol is bad for you, high blood pressure is the precursor to heart attacks. Low 25D means you don’t have enough sunlight, sore joints mean you need the pharmaceutical DMSO, and low energy means low B-12. It is a story to sell you drugs that change arbitrary markers that give zero f@$# about your health. That is the system in a nutshell.

What rarely gets discussed with patients is that these drugs do not restore kidney function, improve filtration, or fix whatever caused the pressure rise in the first place. They are overriding the system. They reduce volume, relax vessels, interfere with adrenal signaling, or force the kidneys to handle salt and water differently, whether or not that makes sense for the person in front of you.
At first, everything looks fine. The cuff reads lower. The chart looks better. Everyone relaxes. Meanwhile, the body is still dealing with the same filtration problem it had before, except now it has less force to work with. So it compensates the only way it knows how. It tightens elsewhere. It shifts electrolytes. It activates backup hormone systems. This is why one blood pressure medication quietly turns into two, then three, then a higher dose, then another add-on diuretic “just to help.”
Anyone who has actually followed patients long enough has seen this pattern. Meaning every single cardiologist knows they are making the problem eventually worse, for the brief period they could still lie to themselves and believe they are helping. The swelling starts. The fatigue deepens. Labs drift in the wrong direction, slowly enough that no single visit feels alarming. When kidney numbers worsen, it’s blamed on age, bad luck, or “progression,” not on years of interfering with the pressure that kept filtration barely functional. Just a brief glance at the 1000’s of patients progressing in the same horrific manner due to the drugs prescribed is beyond obvious. Yes, folks, I hate to break it to you, but the Md’s know exactly what he or she is doing.
By the time the MIC’s wet dream of extremely profitable dialysis is introduced, the story has already been rewritten. The medications are treated as life-saving and necessary. The kidney failure is treated as inevitable and unrelated to the blood pressure drugs and their effects. No one goes back to the beginning and asks whether suppressing a compensatory signal for years might have played a role in where the patient ended up.
I may not be the sharpest tool in the shed, but even I can add 1+1 and get 2. And I haven’t sold my soul to poison people for a dollar either, unlike some people:

(Dr. Andrew Kaufman on Instagram)
Influencers, Protocols, and the Same Old Mistake in New Packaging
Once people realize something is wrong with the blood pressure story, they go looking for answers. That instinct is correct. Where it goes sideways is in what comes next.
Influencers thrive in this space because they speak to a real frustration. Patients sense that suppressing a number has not made them healthier. They feel worse, not better. They see swelling, fatigue, and declining kidney function, and they are told this is normal, inevitable, or unrelated. When someone online says, “They’re missing the root cause,” it lands because it’s true.
This is where the classic 80/20 rule comes in.
The influencer gives you eighty percent truth, enough to earn your trust, enough to make you feel seen, enough to confirm that something is deeply wrong with the official story. And then the remaining twenty percent quietly kicks you in the shins. That last piece is where substances get introduced, protocols get sold, and pressure gets chased all over again under a different name.
Ignorance is not an excuse here. If you recommend something for profit, you have a responsibility to understand exactly what that substance is doing in the body, not how much it improves your bank account. Good intentions do not protect kidneys. Confidence does not restore filtration.
The problem is that most influencers stop one step short of understanding what the root actually is.
They still chase the pressure and want to INTERFERE with the extremely sensitive pressure gauge and change the pressure. That is like seeing the engine light come on, covering it with duct tape, and patting yourself on the back for replacing the radiator fluid. You didn’t address the real problem. And now we have even bigger problems.
Whether it’s framed as natural, holistic, ancestral, or biohacked, the move is the same. Change the number. Relax the vessels. Shift fluids. Force electrolyte movement. Drink more water. Silence the signal and call it a cure.
Figures like Thomas Cowan and Andrew Kaufman position themselves as critics of institutional medicine, and in some narrow respects, they are. They correctly sense that blood pressure is being misunderstood. They correctly challenge the idea that a cuff reading represents a disease. That part is useful, as exemplified above.
That is also where it should stop.
Both ultimately fall into the same trap they claim to be opposing. They replace pharmaceutical authority with personal authority and then sell certainty in the form of substances, protocols, or even black-box interventions like coffee-castor oil-turpentine enemas, methylene blue, and a fixation on specific compounds framed as solutions. Different packaging. Same mistake: it is a cardiac root; it is a renal loop to address.
Changing pressure is not the solution. It is, however, the nail in the coffin.
Dialysis does not care whether pressure was lowered with a prescription, a supplement, drinking excess water, or an influencer-approved protocol. When filtration fails long enough, the outcome is the same. Waste accumulates. Electrolytes destabilize. Fluid backs up. The body compensates until it can no longer.
Some influencers are right about what is broken. Many are wrong about how to fix it. Separating insight from prescription is not optional here. It is survival.
Stop Treating the Sound and Listen to the Message
What we measure in the arm is not a moral failure of the heart. It is pressure generated by the kidneys to filter blood, regulate electrolytes, and maintain homeostasis of the internal environment. When that pressure is treated as the enemy, the very force keeping filtration alive is stripped away.
This article is not an argument against medicine, nor is it an argument for doing nothing. It is an argument for asking the right question. Not how low can we push the number, but why does this body need this pressure right now, and what would allow it to regulate itself again? Meaning, what can we subtract so the body can once again fall back into homeostasis? The influencers add because that is where their money lies.
If the sound of pressure is treated as the root problem, the system will continue to fail.
Why the Dialysis Stories Matter
I included stories about dialysis for a reason. Not for shock value or to scare people, but because after nearly four decades working in “medicine”, I occupy a strange position that most people never see from. I don’t just meet patients at the beginning of their diagnosis. I meet them at the end of the road.
I see people after years and decades of doing what they were told to do. They took the medications. They lowered the numbers. They trusted that controlling blood pressure meant controlling risk. And yet, many of them still arrive at dialysis with bodies swollen with fluid, exhausted hearts, failing kidneys, and a sense of disbelief that this is where everything led. One particular patient always had very high pressures, 180/100, and it was a trick to get them down. When she finally agreed to go to hospice and went off all of her medications, the statin drugs, the 3 blood pressure drugs, the blood thinner, and gabapentin, her pressures were low, 128/84 was the first one, then the subsequent visits were 120/74, 116/59, and stayed there. This happens over and over after they go off the drugs. First, it stays high, and then it drops to “acceptable” levels. Just in time to eke out the last dollar for care before they die.
From one angle, this is a disadvantage. It means witnessing the slow, quiet accumulation of devastation. From another angle, it is an advantage, because patterns become impossible to ignore when you see the long arc instead of isolated moments. You start to recognize that what looks like success early on does not translate into resilience later. And it goes without saying, if I can see it, so can everyone else. The hospice MD laughed about why her 110-year-old patient was suddenly getting better after getting into hospice. “Because we took him off the drugs” lol lol lol “…and now we have to take him off hospice because he is fine” lol lol lol. I don’t find it funny. Not in the slightest.
Dialysis is often treated as an unfortunate but unavoidable outcome, the natural progression of disease. In reality, it represents the point at which the kidneys can no longer perform their most basic function: filtering the blood well enough to sustain life. Reaching that point is rarely sudden. It is usually the result of years of strain, compensation, and missed opportunities to address root causes.
This is why this article goes further than the first two. Those pieces focused on reframing how we think about blood vs kidney pressure and kidney function. This one asks a harder question: what happens when we rely primarily on medications to manage a signal, while leaving diet, movement, stress, and daily habits largely untouched? The idea that there is a pill for every ill is standard operating procedure in ANY medical setting, allopathic or functional.
We Know the Kidneys Are Failing
To understand why kidney function matters so much, we have to be clear about what the kidneys are actually responsible for removing from the body.
Metabolic waste is produced in very specific, ordinary ways. When muscles contract, they burn fuel to create movement, and that process generates byproducts like creatinine. When we eat food, especially protein, the body breaks it down into amino acids to build and repair tissue. What the body cannot use gets converted into nitrogen-based waste, primarily urea. Every heartbeat, every step, every meal adds more of these waste products into the bloodstream, which must be cleared before serious effects begin to develop.
This waste enters the blood because the blood is the transport system. It carries nutrients to cells but also carries away the byproducts of metabolism. As long as we are alive and breathing, waste is continuously dumped into circulation. There is no off switch. The only way to prevent these substances from building up to toxic levels is constant filtration by the kidneys.
The most important metabolic wastes include ammonia and urea from protein metabolism, creatinine from muscle activity, uric acid from the breakdown of genetic material, excess electrolytes like potassium and phosphorus, and acidic compounds that would otherwise alter blood pH. These substances cannot remain in the bloodstream indefinitely or you will die.
We know these wastes exist because we can measure them and do so constantly with dialysis. Blood tests rise when filtration slows. Urine contains them when filtration is working. Urine is not a random fluid loss. It is evidence that the kidneys are functioning properly. Its composition tells us what has been successfully removed from circulation. Which is just one of the smoking guns for why you should NEVER drink urine.
When the kidneys begin to fail, this process breaks down quickly. Waste accumulates. Fluid is retained. Blood volume increases. Fluid leaves blood vessels and enters tissues, causing swelling in the legs, abdomen, and lungs. This is why people with kidney failure look like they are filling up with water. Without adequate filtration, this progression does not take years. People who stop clearing metabolic waste do not slowly decline. They become critically ill within weeks. Dialysis exists for one reason only: to replace kidney filtration when the body can no longer do it on its own and keep the person alive and chained to the for-profit machines.
One of the earliest and most important signs that kidney filtration is impaired is the presence of protein in the urine. Under normal conditions, protein molecules are too large to pass through the kidney’s filtration barrier. When protein appears in the urine, it means that the barrier has been compromised. Proteinuria is not a lab quirk. It is a structural warning. It tells us that the kidney is no longer filtering cleanly and that the system is under strain.
Kidney disease is not diagnosed by a single moment or number. It is recognized through patterns: rising waste markers, protein loss in urine, fluid retention, and declining resilience. These changes reflect a system that is being pushed beyond its capacity to maintain balance.
This is the foundation. Before talking about medications, pressure, or long-term outcomes, it has to be clear what is at stake. The kidneys are not optional accessories. They are the body’s primary defense against internal toxicity. When that defense weakens, everything else follows.
Fixed Kidney Load, Reduced Force
The kidneys do not passively accept whatever blood flow they receive. They require a continuously adjustable pressure range to filter blood effectively, because the amount of waste in the blood is constantly changing.
That pressure is generated by the heart and delivered through the arterial system.
When the heart contracts, it creates the force that pushes blood through the kidney’s filtration units. If that force is reduced, less blood is filtered per unit of time. Filtration slows. Waste begins to accumulate in the bloodstream. The kidneys sense this immediately.
What matters here is not the number on a blood pressure cuff, but the pressure at the level of the kidney filters. Lowering the heart’s ability to generate force lowers filtration pressure unless something else changes to compensate.
So when pressure drops, the kidneys respond by compensating internally.
They adjust resistance within the kidney itself. Blood vessels feeding the filters are narrowed or widened to redirect pressure. Blood flow is redistributed to favor filtration over other functions. Hormonal systems are leaned on more heavily to preserve enough force to keep filtration going.
In the short term, this works. Filtration is preserved. Blood tests may remain stable. There is no immediate failure.
But the workload has not been reduced. It has been shifted.
Instead of being carried by the broader circulatory system, a greater burden is transferred to smaller, more fragile structures within the kidney. Filtration is achieved by squeezing performance out of the system rather than allowing it to operate under relaxed conditions.
Over time, this becomes the default operating state. Chronic UTI’s, kidney stones, more frequent urination, lower flank and back aches can be initial signs of kidney stress.
Structures designed to function across a wide range of pressures are held in a narrowed range. The filters experience higher localized stress even though overall blood pressure appears lower. The system loses flexibility. It becomes less tolerant of dehydration, illness, heat, stress, and changes in medication.
This is why lowering blood pressure is never protective for the kidneys. It depends entirely on whether the underlying load has been reduced.
Blood pressure drugs lower pressure in different ways. Some reduce the force of heart contraction. Some relax blood vessels, so resistance drops. Some reduce circulating volume. Some interfere with signaling systems that normally raise pressure. The details differ, but the outcome is the same: less force is delivered to the kidneys.
What does not change is the amount of waste that must still be filtered.
This is the mismatch.
Blood pressure drugs do not reduce the kidneys’ workload. They reduce the force available to meet that workload. The kidney makes up the difference through chronic internal compensation, which drives long-term damage.
Nothing about this requires the drugs to be toxic. Nothing requires bad intentions. Nothing requires dramatic early failure.
It is simply a system being asked to do the same job under constrained conditions for too long. “Once you understand this mismatch, the next question becomes unavoidable: what increases the load in the first place?”

If you appreciate Medicine Girl's research, please consider hooking her up with a coffee or making a Ko-Fi donation.







![BLOOD PRESSURED TO DEATH: How to DESTROY Your Kidneys in 5 Easy Steps [Part 1 of 3]](https://dropinblog.net/cdn-cgi/image/fit=scale-down,format=auto,width=700/34264201/files/featured/bce83ada-f4c0-4cdb-a4e7-bf4eab08bb07-1280x720.webp)



![Mag-Naus-Eum: The Metal You’ve Been Drinking [Part 2]](https://dropinblog.net/cdn-cgi/image/fit=scale-down,format=auto,width=700/34264201/files/featured/mg-mg-part-2.jpg)
![The Great Magnesium Poisoning [Part 1]](https://dropinblog.net/cdn-cgi/image/fit=scale-down,format=auto,width=700/34264201/files/featured/mg-mg-2.png)

![Bringing Up The Underworld: Vivisection and Organ Donation [Cannibals Part 4]](https://dropinblog.net/cdn-cgi/image/fit=scale-down,format=auto,width=700/34264201/files/featured/4aad8890-f8f1-4198-910c-e85a0171247c-1280x720.webp)




